DESCOVY Film-coated tablet Ref.[10515] Active ingredients: Emtricitabine Emtricitabine and Tenofovir alafenamide Tenofovir alafenamide
Source: European Medicines Agency (EU) Revision Year: 2023 Publisher: Gilead Sciences Ireland UC, Carrigtohill, County Cork, T45 DP77, Ireland
4.3. Contraindications
Hypersensitivity to the active substances or to any of the excipients listed in section 6.1.
4.4. Special warnings and precautions for use
Patients co-infected with HIV and hepatitis B or C virus
Patients with chronic hepatitis B or C treated with antiretroviral therapy are at an increased risk for severe and potentially fatal hepatic adverse reactions.
The safety and efficacy of Descovy in patients co-infected with HIV-1 and hepatitis C virus (HCV) have not been established.
Tenofovir alafenamide is active against hepatitis B virus (HBV). Discontinuation of Descovy therapy in patients co-infected with HIV and HBV may be associated with severe acute exacerbations of hepatitis. Patients co-infected with HIV and HBV who discontinue Descovy should be closely monitored with both clinical and laboratory follow-up for at least several months after stopping treatment.
Liver disease
The safety and efficacy of Descovy in patients with significant underlying liver disorders have not been established (see sections 4.2 and 5.2).
Patients with pre-existing liver dysfunction, including chronic active hepatitis, have an increased frequency of liver function abnormalities during combination antiretroviral therapy (CART) and should be monitored according to standard practice. If there is evidence of worsening liver disease in such patients, interruption or discontinuation of treatment must be considered.
Weight and metabolic parameters
An increase in weight and in levels of blood lipids and glucose may occur during antiretroviral therapy. Such changes may in part be linked to disease control and life style. For lipids, there is in some cases evidence for a treatment effect, while for weight gain there is no strong evidence relating this to any particular treatment. For monitoring of blood lipids and glucose reference is made to established HIV treatment guidelines. Lipid disorders should be managed as clinically appropriate.
Mitochondrial dysfunction following exposure in utero
Nucleos(t)ide analogues may impact mitochondrial function to a variable degree, which is most pronounced with stavudine, didanosine and zidovudine. There have been reports of mitochondrial dysfunction in HIV negative infants exposed in utero and/or postnatally to nucleoside analogues; these have predominantly concerned treatment with regimens containing zidovudine. The main adverse reactions reported are haematological disorders (anaemia, neutropenia) and metabolic disorders (hyperlactatemia, hyperlipasemia). These events have often been transitory. Late onset neurological disorders have been reported rarely (hypertonia, convulsion, abnormal behaviour). Whether such neurological disorders are transient or permanent is currently unknown. These findings should be considered for any child exposed in utero to nucleos(t)ide analogues, who present with severe clinical findings of unknown etiology, particularly neurologic findings. These findings do not affect current national recommendations to use antiretroviral therapy in pregnant women to prevent vertical transmission of HIV.
Immune Reactivation Syndrome
In HIV infected patients with severe immune deficiency at the time of institution of CART, an inflammatory reaction to asymptomatic or residual opportunistic pathogens may arise and cause serious clinical conditions, or aggravation of symptoms. Typically, such reactions have been observed within the first few weeks or months of initiation of CART. Relevant examples include cytomegalovirus retinitis, generalised and/or focal mycobacterial infections, and Pneumocystis jirovecii pneumonia. Any inflammatory symptoms should be evaluated and treatment instituted when necessary.
Autoimmune disorders (such as Graves' disease and autoimmune hepatitis) have also been reported to occur in the setting of immune reactivation; however, the reported time to onset is more variable, and these events can occur many months after initiation of treatment.
Patients with HIV-1 harbouring mutations
Descovy should be avoided in antiretroviral-experienced patients with HIV-1 harbouring the K65R mutation (see section 5.1).
Triple nucleoside therapy
There have been reports of a high rate of virological failure and of emergence of resistance at an early stage when tenofovir disoproxil was combined with lamivudine and abacavir as well as with lamivudine and didanosine as a once daily regimen. Therefore, the same problems may be seen if Descovy is administered with a third nucleoside analogue.
Opportunistic infections
Patients receiving Descovy or any other antiretroviral therapy may continue to develop opportunistic infections and other complications of HIV infection, and, therefore, should remain under close clinical observation by physicians experienced in the treatment of patients with HIV associated diseases.
Osteonecrosis
Although the aetiology is considered to be multifactorial (including corticosteroid use, alcohol consumption, severe immunosuppression, higher body mass index), cases of osteonecrosis have been reported particularly in patients with advanced HIV disease and/or long-term exposure to CART. Patients should be advised to seek medical advice if they experience joint aches and pain, joint stiffness or difficulty in movement.
Nephrotoxicity
Post-marketing cases of renal impairment, including acute renal failure and proximal renal tubulopathy have been reported with tenofovir alafenamide-containing products. A potential risk of nephrotoxicity resulting from chronic exposure to low levels of tenofovir due to dosing with tenofovir alafenamide cannot be excluded (see section 5.3).
It is recommended that renal function is assessed in all patients prior to, or when initiating, therapy with Descovy and that it is also monitored during therapy in all patients as clinically appropriate. In patients who develop clinically significant decreases in renal function, or evidence of proximal renal tubulopathy, discontinuation of Descovy should be considered.
Patients with end stage renal disease on chronic haemodialysis
Descovy should generally be avoided, but may be used in adults with end stage renal disease (estimated CrCl <15 mL/min) on chronic haemodialysis if the potential benefits outweigh the potential risks (see section 4.2). In a study of emtricitabine + tenofovir alafenamide in combination with elvitegravir + cobicistat as a fixed-dose combination tablet (E/C/F/TAF) in HIV-1 infected adults with end stage renal disease (estimated CrCl <15 mL/min) on chronic haemodialysis, efficacy was maintained through 48 weeks but emtricitabine exposure was significantly higher than in patients with normal renal function. Although there were no new safety issues identified, the implications of increased emtricitabine exposure remain uncertain (see sections 4.8 and 5.2).
Co-administration of other medicinal products
The co-administration of Descovy is not recommended with certain anticonvulsants (e.g., carbamazepine, oxcarbazepine, phenobarbital and phenytoin), antimycobacterials (e.g., rifampicin, rifabutin, rifapentine), St. John’s wort and HIV protease inhibitors (PIs) other than atazanavir, lopinavir and darunavir (see section 4.5).
Descovy should not be administered concomitantly with medicinal products containing tenofovir alafenamide, tenofovir disoproxil, emtricitabine, lamivudine or adefovir dipivoxil.
Excipients
This medicine contains less than 1 mmol sodium (23 mg) per tablet, that is to say essentially ‘sodium-free’.
4.5. Interaction with other medicinal products and other forms of interaction
Interaction studies have only been performed in adults.
Descovy should not be administered concomitantly with medicinal products containing tenofovir alafenamide, tenofovir disoproxil, emtricitabine, lamivudine or adefovir dipivoxil.
Emtricitabine
In vitro and clinical pharmacokinetic drug-drug interaction studies have shown that the potential for CYP-mediated interactions involving emtricitabine with other medicinal products is low. Co-administration of emtricitabine with medicinal products that are eliminated by active tubular secretion may increase concentrations of emtricitabine, and/or the co-administered medicinal product. Medicinal products that decrease renal function may increase concentrations of emtricitabine.
Tenofovir alafenamide
Tenofovir alafenamide is transported by P-glycoprotein (P-gp) and breast cancer resistance protein (BCRP). Medicinal products that strongly affect P-gp and BCRP activity may lead to changes in tenofovir alafenamide absorption. Medicinal products that induce P-gp activity (e.g., rifampicin, rifabutin, carbamazepine, phenobarbital) are expected to decrease the absorption of tenofovir alafenamide, resulting in decreased plasma concentration of tenofovir alafenamide, which may lead to loss of therapeutic effect of Descovy and development of resistance. Co-administration of Descovy with other medicinal products that inhibit P-gp and BCRP activity (e.g., cobicistat, ritonavir, ciclosporin) is expected to increase the absorption and plasma concentration of tenofovir alafenamide. Based on data from an in vitro study, co-administration of tenofovir alafenamide and xanthine oxidase inhibitors (e.g., febuxostat) is not expected to increase systemic exposure to tenofovir in vivo.
Tenofovir alafenamide is not an inhibitor of CYP1A2, CYP2B6, CYP2C8, CYP2C9, CYP2C19, or CYP2D6 in vitro. It is not an inhibitor or inducer of CYP3A in vivo. Tenofovir alafenamide is a substrate of OATP1B1 and OATP1B3 in vitro. The distribution of tenofovir alafenamide in the body may be affected by the activity of OATP1B1 and OATP1B3.
Other interactions
Tenofovir alafenamide is not an inhibitor of human uridine diphosphate glucuronosyltransferase (UGT) 1A1 in vitro. It is not known whether tenofovir alafenamide is an inhibitor of other UGT enzymes. Emtricitabine did not inhibit the glucuronidation reaction of a non-specific UGT substrate in vitro.
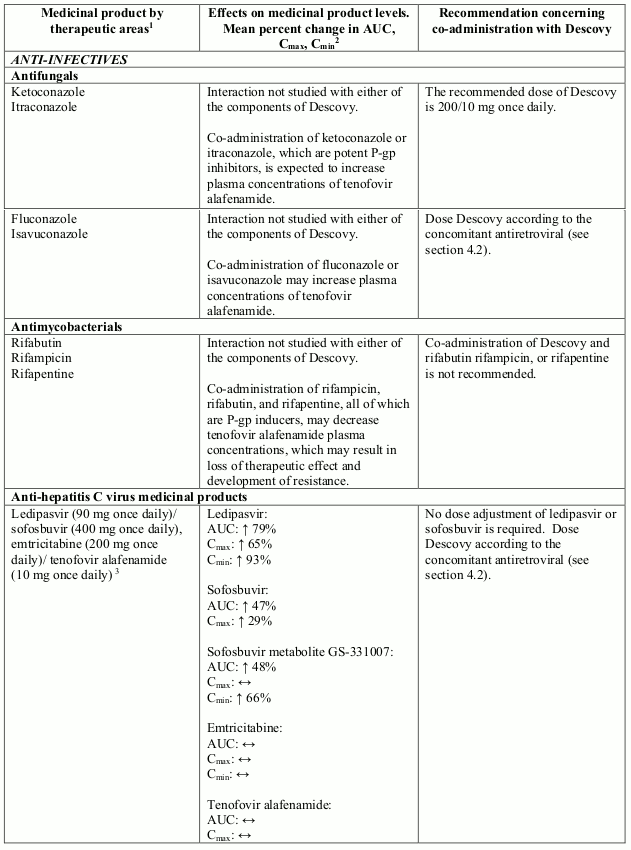
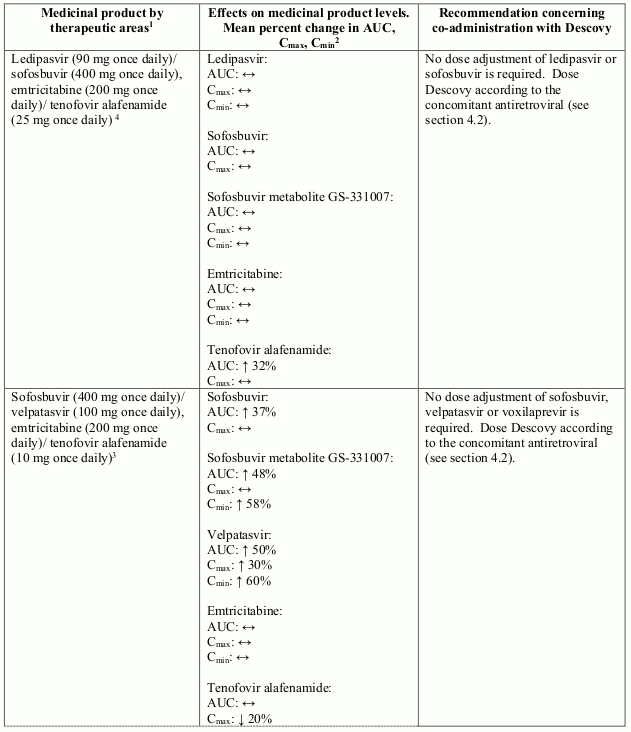
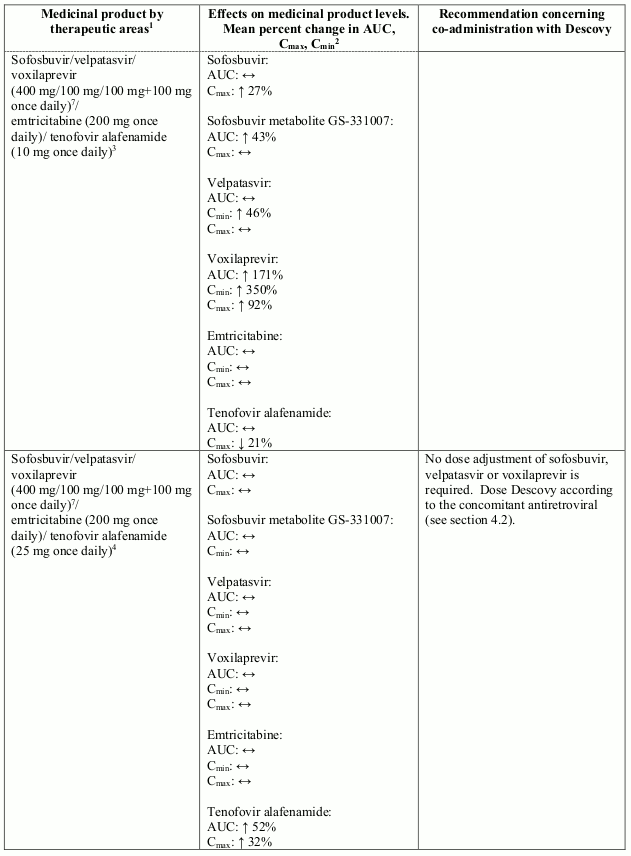
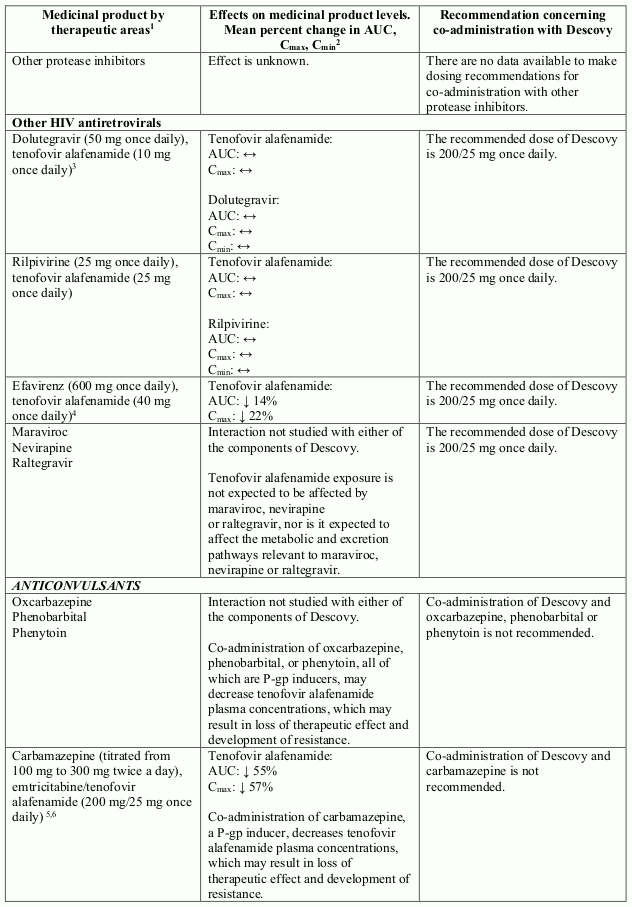
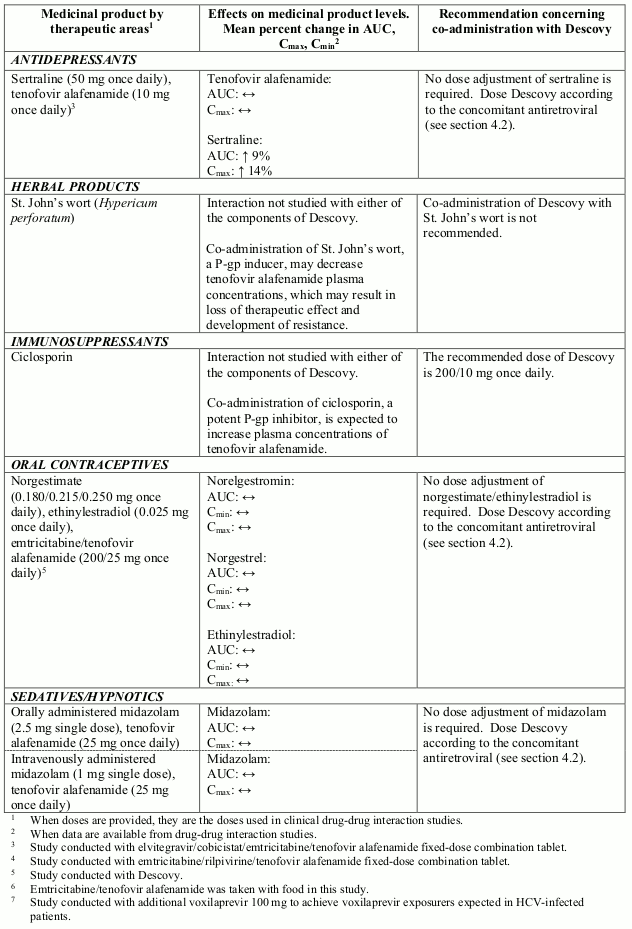
Interactions between the components of Descovy and potential co-administered medicinal products are listed in Table 2 (increase is indicated as “↑”, decrease as “↓”, no change as “↔”). The interactions described are based on studies conducted with Descovy, or the components of Descovy as individual agents and/or in combination, or are potential drug-drug interactions that may occur with Descovy.
Table 2. Interactions between the individual components of Descovy and other medicinal products:
4.6. Fertility, pregnancy and lactation
Pregnancy
There are no adequate and well-controlled studies of Descovy or its components in pregnant women. There are no or limited data (less than 300 pregnancy outcomes) from the use of tenofovir alafenamide in pregnant women. However, a large amount of data on pregnant women (more than 1,000 exposed outcomes) indicate no malformative nor foetal/neonatal toxicity associated with emtricitabine.
Animal studies do not indicate direct or indirect harmful effects of emtricitabine with respect to fertility parameters, pregnancy, foetal development, parturition or postnatal development. Studies of tenofovir alafenamide in animals have shown no evidence of harmful effects on fertility parameters, pregnancy, or foetal development (see section 5.3).
Descovy should be used during pregnancy only if the potential benefit justifies the potential risk to the foetus.
Breast-feeding
It is not known whether tenofovir alafenamide is excreted in human milk. Emtricitabine is excreted in human milk. In animal studies it has been shown that tenofovir is excreted in milk.
There is insufficient information on the effects of emtricitabine and tenofovir in newborns/infants. Therefore, Descovy should not be used during breast-feeding.
In order to avoid transmission of HIV to the infant it is recommended that women living with HIV do not breast-feed their infants.
Fertility
There are no data on fertility from the use of Descovy in humans. In animal studies there were no effects of emtricitabine and tenofovir alafenamide on mating or fertility parameters (see section 5.3).
4.7. Effects on ability to drive and use machines
Descovy may have minor influence on the ability to drive and use machines. Patients should be informed that dizziness has been reported during treatment with Descovy.
4.8. Undesirable effects
Summary of the safety profile
Assessment of adverse reactions is based on safety data from across all Phase 2 and 3 studies in which HIV-1 infected patients received medicinal products containing emtricitabine and tenofovir alafenamide and from post-marketing experience. In clinical studies of treatment-naïve adult patients receiving emtricitabine and tenofovir alafenamide with elvitegravir and cobicistat as the fixed-dose combination tablet elvitegravir 150 mg/cobicistat 150 mg/emtricitabine 200 mg/tenofovir alafenamide (as fumarate) 10 mg (E/C/F/TAF) through 144 weeks, the most frequently reported adverse reactions were diarrhoea (7%), nausea (11%), and headache (6%).
Tabulated summary of adverse reactions
The adverse reactions in Table 3 are listed by system organ class and frequency. Frequencies are defined as follows: very common (≥1/10), common (≥1/100 to <1/10) and uncommon (≥1/1,000 to <1/100).
Table 3. Tabulated list of adverse reactions1:
| Frequency | Adverse reaction |
|---|---|
| Blood and lymphatic system disorders | |
| Uncommon: | anaemia2 |
| Psychiatric disorders | |
| Common: | abnormal dreams |
| Nervous system disorders | |
| Common: | headache, dizziness |
| Gastrointestinal disorders | |
| Very common: | nausea |
| Common: | diarrhoea, vomiting, abdominal pain, flatulence |
| Uncommon: | dyspepsia |
| Skin and subcutaneous tissue disorders | |
| Common: | Rash |
| Uncommon: | angioedema3,4, pruritus, urticaria4 |
| Musculoskeletal and connective tissue disorders | |
| Uncommon: | arthralgia |
| General disorders and administration site conditions | |
| Common: | fatigue |
1 With the exception of angioedema, anaemia and urticaria (see footnotes 2,3 and 4), all adverse reactions were identified from clinical studies of F/TAF containing products. The frequencies were derived from Phase 3 E/C/F/TAF clinical studies in 866 treatment-naïve adult patients through 144 weeks of treatment (GS-US-292-0104 and GS-US-292-0111).
2 This adverse reaction was not observed in the clinical studies of F/TAF-containing products but identified from clinical studies or post-marketing experience for emtricitabine when used with other antiretrovirals.
3 This adverse reaction was identified through post-marketing surveillance for emtricitabine-containing products.
4 This adverse reaction was identified through post-marketing surveillance for tenofovir alafenamide-containing products.
Description of selected adverse reactions
Immune Reactivation Syndrome
In HIV infected patients with severe immune deficiency at the time of initiation of CART, an inflammatory reaction to asymptomatic or residual opportunistic infections may arise. Autoimmune disorders (such as Graves' disease and autoimmune hepatitis) have also been reported; however, the reported time to onset is more variable, and these events can occur many months after initiation of treatment (see section 4.4).
Osteonecrosis
Cases of osteonecrosis have been reported, particularly in patients with generally acknowledged risk factors, advanced HIV disease or long-term exposure to CART. The frequency of this is unknown (see section 4.4).
Changes in lipid laboratory tests
In studies in treatment-naïve patients, increases from baseline were observed in both the tenofovir alafenamide fumarate and tenofovir disoproxil fumarate containing treatment groups for the fasting lipid parameters total cholesterol, direct low-density lipoprotein (LDL)- and high-density lipoprotein (HDL)cholesterol, and triglycerides at Week 144. The median increase from baseline for those parameters was greater in the E/C/F/TAF group compared with the elvitegravir 150 mg/cobicistat 150 mg/emtricitabine 200 mg/tenofovir disoproxil (as fumarate) 245 mg (E/C/F/TDF) group at Week 144 (p<0.001 for the difference between treatment groups for fasting total cholesterol, direct LDL and HDL-cholesterol, and triglycerides). The median (Q1, Q3) change from baseline in total cholesterol to HDL-cholesterol ratio at Week 144 was 0.2 (-0.3, 0.7) in the E/C/F/TAF group and 0.1 (-0.4, 0.6) in the E/C/F/TDF group (p=0.006 for the difference between treatment groups).
In a study of virologically suppressed patients switching from emtricitabine/tenofovir disoproxil fumarate to Descovy while maintaining the third antiretroviral agent (Study GS-US-311-1089), increases from baseline were observed in the fasting lipid parameters total cholesterol, direct LDL cholesterol and triglycerides in the Descovy arm compared with little change in the emtricitabine/tenofovir disproxil fumarate arm (p≤0.009 for the difference between groups in changes from baseline). There was little change from baseline in median fasting values for HDL cholesterol and glucose, or in the fasting total cholesterol to HDL cholesterol ratio in either treatment arm at Week 96. None of the changes was considered clinically relevant.
In a study of virologically suppressed adult patients switching from abacavir/lamivudine to Descovy while maintaining the third antiretroviral agent (Study GS-US-311-1717), there were minimal changes in lipid parameters.
Metabolic parameters
Weight and levels of blood lipids and glucose may increase during antiretroviral therapy (see section 4.4).
Paediatric population
The safety of emtricitabine and tenofovir alafenamide was evaluated through 48 weeks in an openlabel clinical study (GS-US-292-0106) in which HIV-1 infected, treatment-naïve paediatric patients aged 12 to <18 years received emtricitabine and tenofovir alafenamide in combination with elvitegravir and cobicistat as a fixed-dose combination tablet. The safety profile of emtricitabine and tenofovir alafenamide given with elvitegravir and cobicistat in 50 adolescent patients was similar to that in adults (see section 5.1).
Other special populations
Patients with renal impairment
The safety of emtricitabine and tenofovir alafenamide was evaluated through 144 weeks in an open-label clinical study (GS-US-292-0112) in which 248 HIV-1 infected patients who were either treatment-naïve (n=6) or virologically suppressed (n=242) with mild to moderate renal impairment (estimated glomerular filtration rate by Cockcroft-Gault method [eGFRCG]: 30-69 mL/min) received emtricitabine and tenofovir alafenamide in combination with elvitegravir and cobicistat as a fixed-dose combination tablet. The safety profile in patients with mild to moderate renal impairment was similar to that in patients with normal renal function (see section 5.1).
The safety of emtricitabine and tenofovir alafenamide was evaluated through 48 weeks in a single arm, open-label clinical study (GS-US-292-1825) in which 55 virologically suppressed HIV-1 infected patients with end stage renal disease (eGFRCG <15 mL/min) on chronic haemodialysis received emtricitabine and tenofovir alafenamide in combination with elvitegravir and cobicistat as a fixed-dose combination tablet. There were no new safety issues identified in patients with end stage renal disease on chronic haemodialysis receiving emtricitabine and tenofovir alafenamide, in combination with elvitegravir and cobicistat as a fixed-dose combination tablet (see section 5.2).
Patients co-infected with HIV and HBV
The safety of emtricitabine and tenofovir alafenamide in combination with elvitegravir and cobicistat as a fixed-dose combination tablet (elvitegravir/cobicistat/emtricitabine/tenofovir alafenamide [E/C/F/TAF]) was evaluated in 72 HIV/HBV co-infected patients receiving treatment for HIV in an open-label clinical study (GS-US-292-1249), through Week 48, in which patients were switched from another antiretroviral regimen (which included tenofovir disoproxil fumarate [TDF] in 69 of 72 patients) to E/C/F/TAF. Based on these limited data, the safety profile of emtricitabine and tenofovir alafenamide in combination with elvitegravir and cobicistat as a fixed-dose combination tablet, in patients with HIV/HBV co-infection, was similar to that in patients with HIV-1 monoinfection (see section 4.4).
Reporting of suspected adverse reactions
Reporting suspected adverse reactions after authorisation of the medicinal product is important. It allows continued monitoring of the benefit/risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions via the national reporting system listed in Appendix V.
6.2. Incompatibilities
Not applicable.
© All content on this website, including data entry, data processing, decision support tools, "RxReasoner" logo and graphics, is the intellectual property of RxReasoner and is protected by copyright laws. Unauthorized reproduction or distribution of any part of this content without explicit written permission from RxReasoner is strictly prohibited. Any third-party content used on this site is acknowledged and utilized under fair use principles.