SELARSDI Solution for injection Ref.[109631] Active ingredients: Ustekinumab
Source: FDA, National Drug Code (US) Revision Year: 2024
12.1. Mechanism of Action
Ustekinumab products are human IgG1қ monoclonal antibodies that bind with specificity to the p40 protein subunit used by both the IL-12 and IL-23 cytokines. IL-12 and IL-23 are naturally occurring cytokines that are involved in inflammatory and immune responses, such as natural killer cell activation and CD4+ T-cell differentiation and activation. In in vitro models, ustekinumab products were shown to disrupt IL-12 and IL-23 mediated signaling and cytokine cascades by disrupting the interaction of these cytokines with a shared cellsurface receptor chain, IL-12Rβ1.
12.2. Pharmacodynamics
Plaque Psoriasis
In a small exploratory trial, a decrease was observed in the expression of mRNA of its molecular targets IL-12 and IL-23 in lesional skin biopsies measured at baseline and up to two weeks post-treatment in subjects with plaque psoriasis.
12.3. Pharmacokinetics
Absorption
In adult subjects with plaque psoriasis, the median time to reach the maximum serum concentration (Tmax) was 13.5 days and 7 days, respectively, after a single subcutaneous administration of 45 mg (N=22) and 90 mg (N=24) of ustekinumab. In healthy subjects (N=30), the median Tmax value (8.5 days) following a single subcutaneous administration of 90 mg of ustekinumab was comparable to that observed in subjects with plaque psoriasis.
Following multiple subcutaneous doses of ustekinumab in adult subjects with plaque psoriasis, steady-state serum concentrations of ustekinumab were achieved by Week 28. The mean (±SD) steady-state trough serum ustekinumab concentrations were 0.69 ± 0.69 mcg/mL for patients less than or equal to 100 kg receiving a 45 mg dose and 0.74 ± 0.78 mcg/mL for patients greater than 100 kg receiving a 90 mg dose. There was no apparent accumulation in serum ustekinumab concentration over time when given subcutaneously every 12 weeks.
Distribution
Population pharmacokinetic analyses showed that the volume of distribution of ustekinumab in the central compartment was 2.7 L (95% CI: 2.69, 2.78) in patients with one indication and 3.0 L (95% CI: 2.96, 3.07) in patients with another indication. The total volume of distribution at steady-state was 4.6 L in patients with one indication and 4.4 L in patients with another indication.
Elimination
The mean (±SD) half-life ranged from 14.9 ± 4.6 to 45.6 ± 80.2 days across all plaque psoriasis trials following subcutaneous administration.
Metabolism
The metabolic pathway of ustekinumab products have not been characterized. As a human IgG1κ monoclonal antibody, ustekinumab products are expected to be degraded into small peptides and amino acids via catabolic pathways in the same manner as endogenous IgG.
Specific Populations
Weight
When given the same dose, subjects with plaque psoriasis or psoriatic arthritis weighing more than 100 kg had lower median serum ustekinumab concentrations compared with those subjects weighing 100 kg or less. The median trough serum concentrations of ustekinumab in subjects of higher weight (greater than 100 kg) in the 90 mg group were comparable to those in subjects of lower weight (100 kg or less) in the 45 mg group.
Age: Geriatric Population
A population pharmacokinetic analysis (N=106/1937 patients with plaque psoriasis greater than or equal to 65 years old) was performed to evaluate the effect of age on the pharmacokinetics of ustekinumab. There were no apparent changes in pharmacokinetic parameters (clearance and volume of distribution) in subjects older than 65 years old.
Age: Pediatric Population
Following multiple recommended doses of ustekinumab in pediatric subjects 6 to 17 years of age with plaque psoriasis, steady-state serum concentrations of ustekinumab were achieved by Week 28. At Week 28, the mean ±SD steady-state trough serum ustekinumab concentrations were 0.36 ± 0.26 mcg/mL and 0.54 ± 0.43 mcg/mL, respectively, in pediatric subjects 6 to 11 years of age and pediatric subjects 12 to 17 years of age.
Overall, the observed steady-state ustekinumab trough concentrations in pediatric patients with plaque psoriasis were within the range of those observed for adult patients with plaque psoriasis and adult patients with PsA after administration of ustekinumab.
Drug Interaction Studies
The effects of IL-12 or IL-23 on the regulation of CYP450 enzymes were evaluated in an in vitro study using human hepatocytes, which showed that IL-12 and/or IL-23 at levels of 10 ng/mL did not alter human CYP450 enzyme activities (CYP1A2, 2B6, 2C9, 2C19, 2D6, or 3A4). However, the clinical relevance of in vitro data has not been established [see Drug Interactions (7.3)].
No in vivo drug interaction studies have been conducted with ustekinumab products.
Population pharmacokinetic analyses indicated that the clearance of ustekinumab was not impacted by concomitant MTX, NSAIDs, and oral corticosteroids, or prior exposure to a TNF blocker in patients with psoriatic arthritis.
13.1. Carcinogenesis, Mutagenesis, Impairment of Fertility
Animal studies have not been conducted to evaluate the carcinogenic or mutagenic potential of ustekinumab products. Published literature showed that administration of murine IL-12 caused an anti-tumor effect in mice that contained transplanted tumors and IL-12/IL-23p40 knockout mice or mice treated with anti-IL-12/IL-23p40 antibody had decreased host defense to tumors. Mice genetically manipulated to be deficient in both IL-12 and IL-23 or IL-12 alone developed UV-induced skin cancers earlier and more frequently compared to wild-type mice. The relevance of these experimental findings in mouse models for malignancy risk in humans is unknown.
No effects on fertility were observed in male cynomolgus monkeys that were administered ustekinumab at subcutaneous doses up to 45 mg/kg twice weekly (45 times the MRHD on a mg/kg basis) prior to and during the mating period. However, fertility and pregnancy outcomes were not evaluated in mated females.
No effects on fertility were observed in female mice that were administered an analogous IL-12/IL-23p40 antibody by subcutaneous administration at doses up to 50 mg/kg, twice weekly, prior to and during early pregnancy.
13.2. Animal Toxicology and/or Pharmacology
In a 26-week toxicology study, one out of 10 monkeys subcutaneously administered 45 mg/kg ustekinumab twice weekly for 26 weeks had a bacterial infection.
14. Clinical Studies
14.1 Adult Plaque Psoriasis
Two multicenter, randomized, double-blind, placebo-controlled trials (Ps STUDY 1 and Ps STUDY 2) enrolled a total of 1996 subjects 18 years of age and older with plaque psoriasis who had a minimum body surface area involvement of 10%, and Psoriasis Area and Severity Index (PASI) score ≥12, and who were candidates for phototherapy or systemic therapy. Subjects with guttate, erythrodermic, or pustular psoriasis were excluded from the trials.
Ps STUDY 1 enrolled 766 subjects and Ps STUDY 2 enrolled 1230 subjects. The trials had the same design through Week 28. In both trials, subjects were randomized in equal proportion to placebo, 45 mg or 90 mg of ustekinumab. Subjects randomized to ustekinumab received 45 mg or 90 mg doses, regardless of weight, at Weeks 0, 4, and 16. Subjects randomized to receive placebo at Weeks 0 and 4 crossed over to receive ustekinumab (either 45 mg or 90 mg) at Weeks 12 and 16.
In both trials, subjects in all treatment groups had a median baseline PASI score ranging from approximately 17 to 18. Baseline PGA score was marked or severe in 44% of subjects in Ps STUDY 1 and 40% of subjects in Ps STUDY 2. Approximately two-thirds of all subjects had received prior phototherapy, 69% had received either prior conventional systemic or biologic therapy for the treatment of psoriasis, with 56% receiving prior conventional systemic therapy and 43% receiving prior biologic therapy. A total of 28% of subjects had a history of psoriatic arthritis.
In both trials, the endpoints were the proportion of subjects who achieved at least a 75% reduction in PASI score (PASI 75) from baseline to Week 12 and treatment success (cleared or minimal) on the Physician’s Global Assessment (PGA). The PGA is a 6-category scale ranging from 0 (cleared) to 5 (severe) that indicates the physician’s overall assessment of psoriasis focusing on plaque thickness/induration, erythema, and scaling.
Clinical Response
The results of Ps STUDY 1 and Ps STUDY 2 are presented in Table 4 below.
Table 4. Clinical Outcomes at Week 12 in Adults with Plaque Psoriasis in Ps STUDY 1 and Ps STUDY 2:
| Ps STUDY 1 Ustekinumab | Ps STUDY 2 Ustekinumab | |||||
|---|---|---|---|---|---|---|
| Placebo | 45 mg | 90 mg | Placebo | 45 mg | 90 mg | |
| Subjects randomized | 255 | 255 | 256 | 410 | 409 | 411 |
| PASI 75 response | 8 (3%) | 171 (67%) | 170 (66%) | 15 (4%) | 273 (67%) | 311 (76%) |
| PGA of Cleared or Minimal | 10 (4%) | 151 (59%) | 156 (61%) | 18 (4%) | 277 (68%) | 300 (73%) |
Examination of age, gender, and race subgroups did not identify differences in response to ustekinumab among these subgroups.
In subjects who weighed 100 kg or less, response rates were comparable with both the 45 mg and 90 mg doses; however, in subjects who weighed greater than 100 kg, higher response rates were seen with 90 mg dosing compared with 45 mg dosing (Table 5 below).
Table 5. Clinical Outcomes by Weight Ps STUDY 1 and Ps STUDY 2:
| Ps STUDY 1 Ustekinumab | Ps STUDY 2 Ustekinumab | |||||
|---|---|---|---|---|---|---|
| Placebo | 45 mg | 90 mg | Placebo | 45 mg | 90 mg | |
| Subjects randomized | 255 | 255 | 256 | 410 | 409 | 411 |
| PASI 75 response | ||||||
| ≤100 kg | 4% 6/166 | 74% 124/168 | 65% 107/164 | 4% 12/290 | 73% 218/297 | 78% 225/289 |
| >100 kg | 2% 2/89 | 54% 47/87 | 68% 63/92 | 3% 3/120 | 49% 55/112 | 71% 86/121 |
| PGA of Cleared or Minimal* | ||||||
| ≤100 kg | 4% 7/166 | 64% 108/168 | 63% 103/164 | 5% 14/290 | 74% 220/297 | 75% 216/289 |
| >100 kg | 3% 3/89 | 49% 43/87 | 58% 53/92 | 3% 4/120 | 51% 57/112 | 69% 84/121 |
* Patients were dosed with trial medication at Weeks 0 and 4.
Subjects in Ps STUDY 1 who were PASI 75 responders at both Weeks 28 and 40 were re-randomized at Week 40 to either continued dosing of ustekinumab (ustekinumab at Week 40) or to withdrawal of therapy (placebo at Week 40). At Week 52, 89% (144/162) of subjects re-randomized to ustekinumab treatment were PASI 75 responders compared with 63% (100/159) of subjects re-randomized to placebo (treatment withdrawal after Week 28 dose). The median time to loss of PASI 75 response among the subjects randomized to treatment withdrawal was 16 weeks.
14.2 Pediatric Plaque Psoriasis
A multicenter, randomized, double blind, placebo-controlled trial (Ps STUDY 3) enrolled 110 pediatric subjects 12 to 17 years of age with a minimum BSA involvement of 10%, a PASI score greater than or equal to 12, and a PGA score greater than or equal to 3, who were candidates for phototherapy or systemic therapy and whose disease was inadequately controlled by topical therapy.
Subjects were randomized to receive placebo (n = 37), the recommended dose of ustekinumab (n = 36), or onehalf the recommended dose of ustekinumab (n = 37) by subcutaneous injection at Weeks 0 and 4 followed by dosing every 12 weeks (q12w). The recommended dose of ustekinumab was 0.75 mg/kg for subjects weighing less than 60 kg, 45 mg for subjects weighing 60 kg to 100 kg, and 90 mg for subjects weighing greater than 100 kg. At Week 12, subjects who received placebo were crossed over to receive ustekinumab at the recommended dose or one-half the recommended dose.
Of the pediatric subjects, approximately 63% had prior exposure to phototherapy or conventional systemic therapy and approximately 11% had prior exposure to biologics.
The endpoints were the proportion of subjects who achieved a PGA score of cleared (0) or minimal (1), PASI 75, and PASI 90 at Week 12. Subjects were followed for up to 60 weeks following first administration of trial agent.
Clinical Response
The efficacy results at Week 12 for Ps STUDY 3 are presented in Table 6.
Table 6. Efficacy Results at Week 12 in the Pediatric Subjects 12 to 17 years with Plaque Psoriasis in Ps Study 3:
| Ps STUDY 3 | ||
|---|---|---|
| Placebo n (%) | Ustekinumab* n (%) | |
| N | 37 | 36 |
| PGA | ||
| PGA of cleared (0) or minimal (1) | 2 (5.4%) | 25 (69.4%) |
| PASI | ||
| PASI 75 responders | 4 (10.8%) | 29 (80.6%) |
| PASI 90 responders | 2 (5.4%) | 22 (61.1%) |
* Using the weight-based dosage regimen specified in Table 1.
14.3 Psoriatic Arthritis
The safety and efficacy of ustekinumab was assessed in 927 patients (PsA STUDY 1, n=615; PsA STUDY 2, n=312), in two randomized, double-blind, placebo-controlled trials in adult patients 18 years of age and older with active PsA (≥5 swollen joints and ≥5 tender joints) despite non-steroidal anti-inflammatory (NSAID) or disease modifying antirheumatic (DMARD) therapy. Patients in these trials had a diagnosis of PsA for at least 6 months. Patients with each subtype of PsA were enrolled, including polyarticular arthritis with the absence of rheumatoid nodules (39%), spondylitis with peripheral arthritis (28%), asymmetric peripheral arthritis (21%), distal interphalangeal involvement (12%) and arthritis mutilans (0.5%). Over 70% and 40% of the patients, respectively, had enthesitis and dactylitis at baseline.
Patients were randomized to receive treatment with ustekinumab 45 mg, 90 mg, or placebo subcutaneously at Weeks 0 and 4 followed by every 12 weeks (q12w) dosing. Approximately 50% of patients continued on stable doses of MTX (≤25 mg/week). The primary endpoint was the percentage of patients achieving ACR 20 response at Week 24.
In PsA STUDY 1 and PsA STUDY 2, 80% and 86% of the patients, respectively, had been previously treated with DMARDs. In PsA STUDY 1, previous treatment with anti-tumor necrosis factor (TNF)-α agent was not allowed. In PsA STUDY 2, 58% (n=180) of the patients had been previously treated with TNF blocker, of whom over 70% had discontinued their TNF blocker treatment for lack of efficacy or intolerance at any time.
Clinical Response
In both trials, a greater proportion of patients achieved ACR 20, ACR 50 and PASI 75 response in the ustekinumab 45 mg and 90 mg groups compared to placebo at Week 24 (see Table 7). ACR 70 responses were also higher in the ustekinumab 45 mg and 90 mg groups, although the difference was only numerical (p=NS) in STUDY 2. Responses were consistent in patients treated with ustekinumab alone or in combination with methotrexate. Responses were similar in patients regardless of prior TNFα exposure.
Table 7. ACR 20, ACR 50, ACR 70 and PASI 75 responses in PsA STUDY 1 and PsA STUDY 2 at Week 24:
| PsA STUDY 1 Ustekinumab | PsA STUDY 2 Ustekinumab | |||||
|---|---|---|---|---|---|---|
| Placebo | 45 mg | 90 mg | Placebo | 45 mg | 90 mg | |
| Number of patients randomized | 206 | 205 | 204 | 104 | 103 | 105 |
| ACR 20 response, N (%) | 47 (23%) | 87 (42%) | 101 (50%) | 21 (20%) | 45 (44%) | 46 (44%) |
| ACR 50 response, N (%) | 18 (9%) | 51 (25%) | 57 (28%) | 7 (7%) | 18 (17%) | 24 (23%) |
| ACR 70 response, N (%) | 5 (2%) | 25 (12%) | 29 (14%) | 3 (3%) | 7 (7%) | 9 (9%) |
| Number of patients with ≥ 3% BSAa | 146 | 145 | 149 | 80 | 80 | 81 |
| PASI 75 response, N (%) | 16 (11%) | 83 (57%) | 93 (62%) | 4 (5%) | 41 (51%) | 45 (56%) |
a Number of patients with ≥ 3% BSA psoriasis skin involvement at baseline
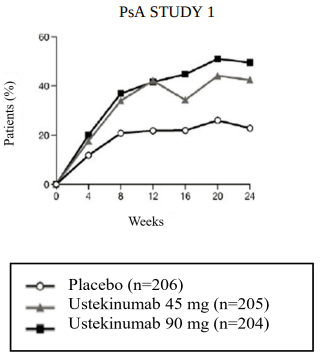
The percent of patients achieving ACR 20 responses by visit is shown in Figure 1.
Figure 1. Percent of patients achieving ACR 20 response through Week 24:
The results of the components of the ACR response criteria are shown in Table 8
Table 8. Mean change from baseline in ACR components at Week 24:
| PsA STUDY 1 Ustekinumab | |||
|---|---|---|---|
| Placebo (N = 206) | 45 mg (N = 205) | 90 mg (N = 204) | |
| Number of swollen jointsa | |||
| Baseline | 15 | 12 | 13 |
| Mean Change at Week 24 | -3 | -5 | -6 |
| Number of tender jointsb | |||
| Baseline | 25 | 22 | 23 |
| Mean Change at Week 24 | -4 | -8 | -9 |
| Patient’s assessment of painc | |||
| Baseline | 6.1 | 6.2 | 6.6 |
| Mean Change at Week 24 | -0.5 | -2.0 | -2.6 |
| Patient global assessmentc | |||
| Baseline | 6.1 | 6.3 | 6.4 |
| Mean Change at Week 24 | -0.5 | -2.0 | -2.5 |
| Physician global assessmentc | |||
| Baseline | 5.8 | 5.7 | 6.1 |
| Mean Change at Week 24 | -1.4 | -2.6 | -3.1 |
| Disability index (HAQ)d | |||
| Baseline | 1.2 | 1.2 | 1.2 |
| Mean Change at Week 24 | -0.1 | -0.3 | -0.4 |
| CRP (mg/dL)e | |||
| Baseline | 1.6 | 1.7 | 1.8 |
| Mean Change at Week 24 | 0.01 | -0.5 | -0.8 |
a Number of swollen joints counted (0-66)
b Number of tender joints counted (0-68)
c Visual analogue scale; 0= best, 10=worst.
d Disability Index of the Health Assessment Questionnaire; 0 = best, 3 = worst, measures the patient’s ability to perform the following: dress/groom, arise, eat, walk, reach, grip, maintain hygiene, and maintain daily activity.
e CRP: (Normal Range 0.0-1.0 mg/dL)
An improvement in enthesitis and dactylitis scores was observed in each ustekinumab group compared with placebo at Week 24.
Physical Function
Ustekinumab-treated patients showed improvement in physical function compared to patients treated with placebo as assessed by HAQ-DI at Week 24. In both trials, the proportion of HAQ-DI responders (≥0.3 improvement in HAQ-DI score) was greater in the ustekinumab 45 mg and 90 mg groups compared to placebo at Week 24.
© All content on this website, including data entry, data processing, decision support tools, "RxReasoner" logo and graphics, is the intellectual property of RxReasoner and is protected by copyright laws. Unauthorized reproduction or distribution of any part of this content without explicit written permission from RxReasoner is strictly prohibited. Any third-party content used on this site is acknowledged and utilized under fair use principles.